Adrenal
Basic Information about the Adrenal Gland:
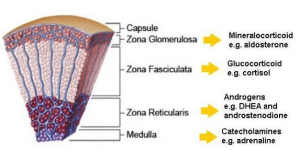
The adrenal glands comprise of an outer cortex with three zones: the glomerulosa (secretes mineralocorticoids), the fasciculata (secretes glucocorticoids) and the reticularis (secretes androgens) as well as the adrenal medulla, which synthesises, stores and secretes catecholamines.
The adrenal hormones affected in Addison’s Disease are the steroid hormones, (the medulla is usually spared). These are grouped into three classes, based on their physiological effects:
Glucocorticoids are so named due to their effect on carbohydrate metabolism. They increase hepatic gluconeogenesis, increase glycogen deposition, increase protein catabolism, affect fat mobilisation, redistribution and deposition, increase blood pressure and stress responses, increase sodium retention and potassium loss, and affect immune function, including lymphocyte inhibition.
Mineralocorticoids: The main mineralocorticoid is aldosterone, which acts on the kidney at the distal convoluted tubule via an intracellular receptor to increase sodium resorption from the urine, and decrease potassium resorption.
Androgens, secreted in a weak form until metabolised in peripheral tissues to testosterone or dihydrotestosterone.
From the Hormone Health Network: www.Hormone.org
The adrenal glands, located at the top of each kidney, produce hormones that help the body control blood sugar, burn protein and fat, react to stressors like a major illness or injury, and regulate blood pressure. Two of the most important adrenal hormones are cortisol and aldosterone. The adrenal glands also produce adrenaline and small amounts of sex hormones called androgens, among other hormones.
Adrenal disorders can be caused by too much or too little of a particular hormone. For example, Cushing syndrome is caused by an overproduction of cortisol, or more commonly, the use of medications called glucocorticoids—cortisol-like drugs—which are used to treat inflammatory disorders such as asthma and rheumatoid arthritis. Untreated Cushing syndrome can lead to diabetes, high blood pressure, and osteoporosis, and other health issues. When the adrenal glands produce too much aldosterone, blood pressure rises. Uncontrolled high blood pressure can put you at risk for stroke, heart attack, heart failure, or kidney failure.
Adrenal insufficiency occurs when the adrenal glands make enough cortisol, and sometimes, aldosterone. Symptoms include fatigue, muscle weakness, decreased appetite, and weight loss. Some people experience nausea, vomiting, and diarrhea. Adrenal insufficiency is treated with hormones that replace the hormones your body is lacking.
A genetic condition called congenital adrenal hyperplasia also causes the adrenal glands to make too little cortisol and/or aldosterone, and too much androgen.
The good news is that the conditions caused by overproduction or underproduction of adrenal hormones are treatable and can keep you healthy over the long-term. Read more about adrenal disorders and treatment and related fact sheets at: Adrenal Gland Disorders on Hormone Health Network.
Congenital Adrenal Hyperplasia
Congenital adrenal hyperplasia (pronounced kuhn-JEN-i-tl uh-DREEN-uhl hahy-per-PLEY-zhuh), or CAH, refers to a group of genetic disorders that affect the adrenal glands. These glands sit on top of the kidneys and release hormones the body needs to function. CAH creates imbalances in these hormones, which cause a wide range of symptoms in infants, children, and adults.
Most commonly, CAH causes male-like characteristics (such as excessive hair growth in girls/women, early hair development in boys) and puberty to occur too early in children. Girls with CAH may be born with ambiguity of their external genitalia, meaning their genitalia do not look like typical female genitalia.
CAH can be categorized as classic or nonclassic. The most common type of CAH can be life-threatening if it is left undiagnosed and untreated in newborns. Most patients with CAH must take daily medications to treat the symptoms. NICHD research aims to find new ways to diagnose and treat the disorder, as well as to help health care providers and scientists better understand how it develops.