Your doctor and/or nutritionist probably has you “carb counting” to help dose your insulin with meals. However, even when you are good with carb counting you are frustrated with the variability in your sugars. Here’s why:

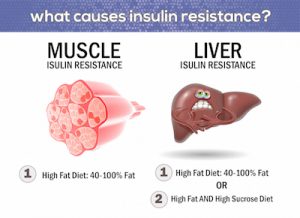
A high fat meal increases the amount of free fatty acids (FFAs) in the blood which causes insulin resistance. You will need more insulin to overcome this insulin resistance FFAs chronically elevated due to repeatedly consuming high fat meals, especially high in saturated fats, is associated with persistent skeletal muscle and liver insulin resistance. This is the same insulin resistance seen with obesity. Protein is slowly broken down and some of it is turned into carbohydrates. The higher the protein load in a meal, the greater impact in your blood sugars hours after a meal. The Glycemic Index (GI), or how rapidly a carbohydrate can impact your blood glucose, can cause a mismatch to the timing of your mealtime insulin peak.
Researches, as reported in the June 2015 issue of Diabetes Care, evaluated the effect of Glycemic Index (GI), protein, and fat composition in meals and effects on post prandial (after the meal) blood sugars in Type 1 Diabetes. They reviewed various studies that used continuous glucose monitoring (CGMS).
The researchers concluded that GI, protein, and fat can drastically affect glucose concentrations in individuals with type 1 diabetes. The effect on three hour postprandial glucose concentrations with the addition of 35 g of fat and 40 g of protein to a meal is equivalent to that resulting from the consumption of 20 g of carbohydrates without insulin. The addition of 50 g of fat to a meal can increase insulin requirements for by greater than two fold.
Study Source: Bell KJ. Impact of Fat, Protein, and Glycemic Index on Postprandial Glucose Control in Type 1 Diabetes: Implications for Intensive Diabetes Management in the Continuous Glucose Monitoring Era. Diabetes Care. June 2015. 38(6)1008-15.